Polysporin Eczema Essentials 1% Hydrocortisone: A review on a hydrocortisone cream over-the-counter
Hydrocortisone cream is a common corticosteroid treatment used for different skin conditions. Depending on the strength, it can exists as a both a prescription and over-the-counter (as a non-prescription product). A popular hydrocortisone cream over-the-counter is Polysporin Eczema Essentials 1% Hydrocortisone cream which is marketed for the treatment of mild eczema.
Fast Fact: Currently in Canada both 0.5% and 1% hydrocortisone cream exist as over-the-counter products (the 0.5% strength has existed as a nonprescription for a long time). In 2014, Health Canada announced that 1% hydrocortisone cream can now be bought without a prescription[1].
Polysporin has always been known for it’s antibiotic line, but it now has an Eczema Essential line with 2 products:
- daily moisturizing cream
- 1% hydrocortisone anti-itch cream
The Polysporin website claims their hydrdocortisone 1% cream can be used to[2]:

- Relieve itch due to eczema flare-ups
- Moisturize to restore visibly healthier skin
- Improve dryness, flaking and redness associated with eczema
What Is Eczema? (Brief Run-Down)
If you are someone that suffers from eczema, you know it is NOT a silent condition! For those of you new to eczema, here are some facts:
Eczema is also known as dermatitis. According to the Canadian Dermatology Association, atopic dermatitis (AD) is the most common type of eczema, and up to 17% of Canadians will experience it in their lives (roughly over 6 million Canadians)[3]. A Quality of Life Report completed by the Eczema Society of Canada found that severe cases of AD can often can negatively affect quality of life[4]. There is still a lot of research to be done because the cause is still unknown and current treatment is not always effective.
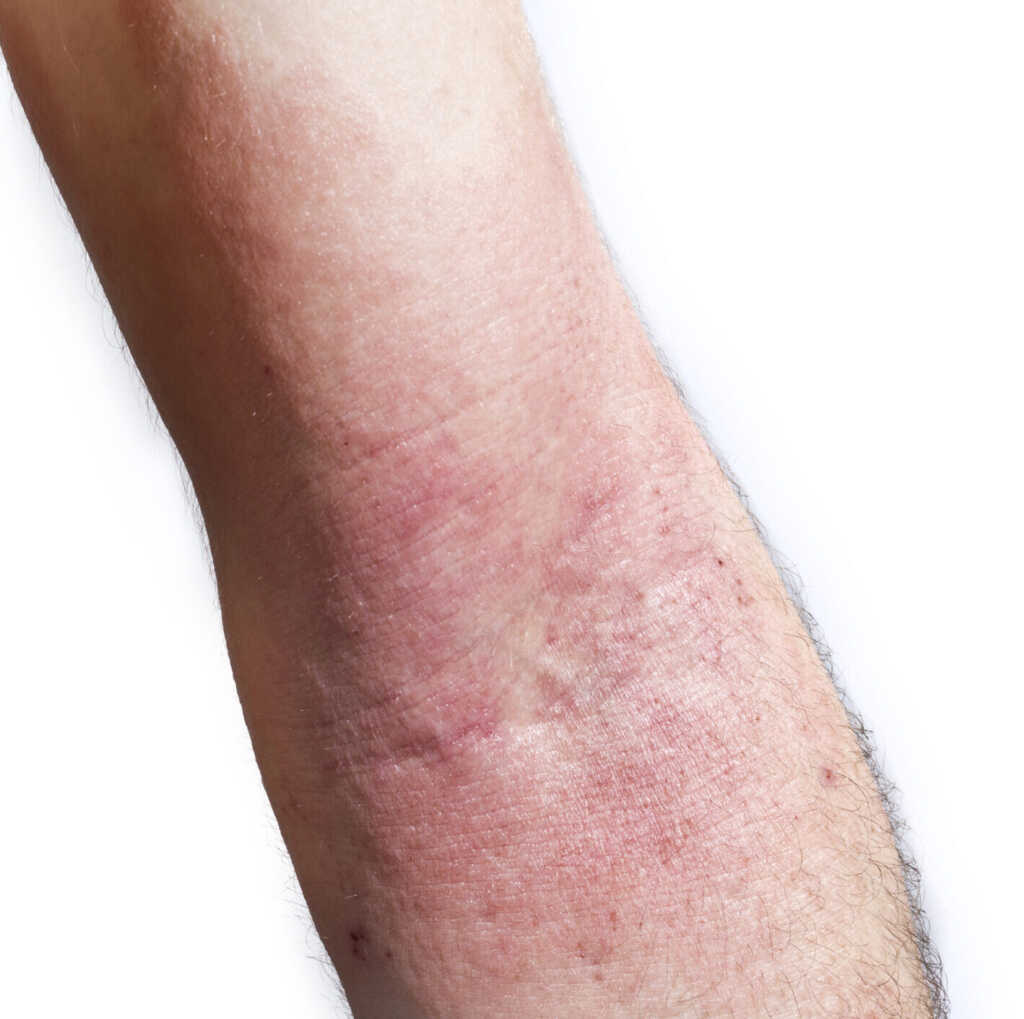
Contact dermatitis (CD) is another common eczema and occurs when you come into something causes skin irritation or an allergic reaction (ie. poison ivy, detergents, harsh soaps, etc.). This is different from AD which as a genetic component and can can often flare-up for a variety of different reasons such as season changes, stress, sweat, bacterial infection[3] . There are other eczemas as well, but AD and CD are the most common,
Atopic Dermatitis (AD): hereditary (has some genetic component) and most common type of eczema
Contact Dermatitis (CD): triggered by touching something that causes an allergy or damage to the skin
One of the most common hallmarks of eczema are insanely itchy patches of red, dry skin. Whether the itch comes first or the rash is still a mystery. Is eczema an ‘itch that rashes’ or the ‘rash that itches’?[5] To make things worse, scratching always worsens itching, and in turn leads to more scratching, creating a seemingly never-ending cycle!
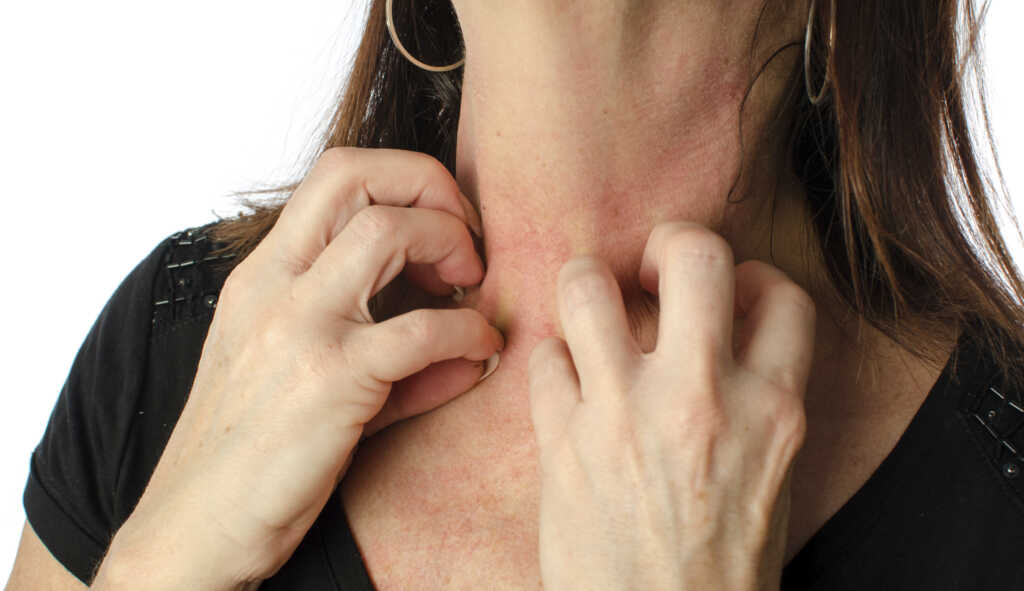
Fast Fact: There are many different types of eczema (chronic inflammatory skin resulting it dry, red and itchy patches). Although the Polysporin Eczema Essentials markets to all eczemas, most of the available evidence for hydrocortisone 1% and corticosteroid use is for atopic dermatitis (AD)
What Topical Treatments Are Used for Eczema?
Topical treatments are treatments you apply (like a cream or ointment) directly onto the top layer of the skin. They are generally used as first-line therapies because they have less side-effects than oral medications[6]. To keep things simple, they can be broken down into three parts:
- Emollients: add moisture back into the skin (can help reduce the itch and need for steroids)
- Anti-inflammatory agents (ie. corticosteroids): help reduce the underlying inflammation of the disease (also helps reduce itch, irritation)
- Anti-itch agents
Emollients and moisturizers are generally tried as the first step before topical corticosteroids are recommended[7].
What Is Polysporin Eczema Essentials 1% Hydrocortisone Cream?
This anti-itch cream as part of the Eczema Essential® line is a topical hydrocortisone cream over-the-counter. The active ingredient hydrocortisone is classified under a group of drugs called corticosteroids, which is the mainstay for anti-inflammatory therapy[7]. The cream is applied topically (directly on the skin) and generally consists of a neutral base (cream) without additional antibiotics.

What Ingredients Are In Polysporin Eczema Essentials 1% Hydrocortisone Cream?
Active Ingredient [2] : hydrocortisone
Other Ingredients [2]: ammonium acryloyldimethyltaurate/vp copolymer, avena sativa (oat) kernel extract, boswellia serrata gum extract, c20-24 olefin, carbomer, ceteareth-6, cetyl alcohol, cis-3-hexenyl salicylate, citric acid, dihydrocitronellol, dimethicone, dipropylene glycol, disodium edta, ethylene brassylate, ethylparaben, glycerin, methylparaben, mineral oil (huile minérale), petrolatum, phenoxyethanol, propylparaben, sodium citrate, sodium hydroxide, stearyl alcohol, vp/eicosene copolymer, water (eau).
What Does Hydrocortisone Cream Do?
When hydrocortisone cream gets absorbed through the skin, it acts on different immune cells to lower or suppress inflammatory processes, while increasing anti-inflammatory responses[8]. This reduction of inflammation is what helps reduce, redness, swelling, and irritation. Along with reducing inflammation, there are also many studies showing they also reduce itch[7].
Does Hydrocortisone 1% Cream Work to Treat Eczema?
Topical steroids (including hydrocortisone 1%) have shown to be effective in treating eczema. For AD specifically, they have been used for over 60 years. There have not been good comparative trials to show whether one corticosteroid is better than another to treat AD so corticosteroids are generally discussed as a group[7].
Topical 1% hydrocortisone (like the one found in Polysporin) is considered one of the lowest potency corticosteroids when compared to 33 other corticosteroids[8]. It is usually considered for treatment in mild to moderate eczema because of it’s low potency. Also, many trials used hydrocortisone 1% in patients experiencing mild to moderate AD. Because there is not strong evidence to pick one corticosteroid over another, other factors are considered such as:
- where the eczema is located
- how severe the eczema is
- personal preference on type of treatment
- cost
- availability
- triggers causing flare-ups
For example, when considering treatment for AD specifically, try and figure out the trigger. If bacteria is triggering a flare-up, the use of an antibiotic mixed with hydrocortisone may help. A small study in children aged 2-15 years found the use of the combination to be effective in treating eczema triggered by a bacteria[9].
More potent corticosteroids are beneficial in severe cases of a disease and disease located on parts of the body where the thin is thicker[10]. Severe eczema may warrant a regimen that is more complex with multiple agents, prescriptions and lifestyle changes. A few studies found tacrolimus to be more effective in moderate to severe eczema but requires a precription from a physician[11],[12].
It is important to remember that moisturizers are essential to the treatment and management of eczema. A number of studies have shown they reduce itching, redness and inflammation due to AD as well as the amount of corticosteroids required[7] .
What Are The Side Effects of Polysporin Eczema Essentials 1% Hydrocortisone?
Again, hydrocortisone 1% is considered as part of the group corticosteroids. Overall, incidents of side effects with topical corticosteroids are generally low when used appropriately[7].
There are greater risks for side effects with:
- stronger (higher-potency) corticosteroids
- applying corticosteroids on thinner skin
- older age
The most common and concerning side effects of topical corticosteroids are:
- burning
- irritation and itchiness
- thinning of the skin
- skin fragility
- stretch marks
- purpura (blood spots)
- spider veins
Low-potency steroids (like hydrocortisone 1%) are the safest agents for longer-term use, treating larger areas, thinner skin and on children. Depending on the severity of the side effects, many of these side effects resolve after discontinuing treatment[12].
Are There Other Safety Concerns With Corticosteroids?
Affected Areas
With any topical corticosteroid, it is always recommended to use it ‘sparingly’ on the affected area. In other words, don’t apply it on normal skin, like you would a moisturizer.
Frequency of Application
It is recommended that most corticosteroids should be applied once or twice daily and using it more often doesn’t necessarily mean better results[10]. This may differ with each person and specific advice from a health care professional working with you. The Polysporin brand advises to apply the hydrocortisone 1% ‘sparingly to the affected area 3-4 times daily’[2].
Duration
Although the brand suggests using for a maximum of 7 days, the duration may vary between individuals depending on their individual factors. According to the Eczema Society of Canada, there should be some improvement after using corticosteroid within a few days and treatment should continue until the redness is gone. They suggest speaking to your doctor if you don’t see any improvement after two weeks[13]. Most corticosteroids should not be used continuously for longer than three months to avoid side effects[10].
Other considerations[2]:
- Do not use on children <2 years or to treat diaper rash (except on the advice of a doctor)
- Do not apply in or around eyes or to large areas
Click here to read a full Q&A with a pharmacist regarding some common safety concerns regarding corticosteroids.
Bottom Line
Eczema, especially AD is challenging to treat. For people over 2 years of age suffering from mild to moderate eczema, Polysporin Eczema Essentials 1% hydrocortisone cream over-the-counter may be helpful if moisturizers are not doing the trick. Use it routinely (ie. two times daily) for a short period of time (1-2 weeks). Discuss longer use with a health care professional to make sure it is safe and appropriate. It is important to see the right medical professional if symptoms worsen or there is no improvement after a few weeks.
Where Can I Buy Polysporin Eczema Essentials 1% Hydrocortisone Cream in Canada?

In Canada, this product can be bought in person from any pharmacy.
Author: Aliya Kassamali, PharmD
Edited and Reviewed by The Health Aisle Team
References:
1. Health Canada. (2014). Hydrocortisone Notice. Retrieved From: https://www.canada.ca/en/health-canada/services/drugs-health-products/drug-products/prescription-drug-list/notice-hydrocortisone.html
2. Polysporin. (2019). Poysporin®. Eczema Essentials®. 1% Hydrocortisone Anti-Itch Cream. Retrieved From: https://www.polysporin.ca/products/eczema-essentials-hydrocortisone-anti-itch-cream
3. Canadian Dermatology Society. Eczema. Retrieved From: https://dermatology.ca/public-patients/skin/eczema/
4. Eczema Society of Canada. (2017). Atopic Dermatitis Quality of Life Report. Retrieved From: https://eczemahelp.ca/resources/
5. Eczema Society of Canada. Managing Eczema. Retrieved From: https://eczemahelp.ca/resources/
6. Hong J, Buddenkotte J., Berger T., et al. Management of Itch in Atopic Dermatitis. (2011). Semin Cutan Med Surg. 30(2): 71–86. doi:10.1016/j.sder.2011.05.002
7. Eichenfield LF, Tom WL, Berger TG, Krol A, Paller AS, Schwarzenberger K, et al. (2014). Guidelines of care for the management of atopic dermatitis: section 2. Management and treatment of atopic dermatitis with topical therapies. J Am Acad Dermatol, 71(1):116-32
8. Draelos, Z.D., Feldman, S.R., Berman, B. et al. (2019). Tolerability of Topical Treatments for Atopic Dermatitis. Dermatol Ther (Heidelb), 9(71): 71-102. https://doi.org/10.1007/s13555-019-0280-7
9. Ramsay C., Savoie J.M, Gilbert M., et al. (1996). The treatment of atopic dermatitis with topical fusidic acid and hydrocortisone acetate. Journal of the European Academy of Dermatology and Venereology. 7(1):S15-S22.
10. Ference JD, Last AR (2009). Choosing Topical Corticosteroids. Am Fam Physician. 2009 Jan 15;79(2):135-4.
11. Reitamo S, Van Leent E., Ho V., et al. (2002). Efficacy and safety of tacrolimus ointment compared with that of hydrocortisone acetate ointment in children with atopic dermatitis. Journal of Allergy and Clinical Immunology, 109(3): 539-546. https://doi.org/10.1067/mai.2002.121831
12. Rahman MF, Nandi AK, Kabir S. et al. (2015). Topical Tacrolimus versus Hydrocortisone on Atopic Dermatitis in Paediatric Patients: A Randomized Controlled Trial. Mymsensingh MedJ, 24(3):457-463.
13. Eczema Society of Canada. Topical Corticosteroids: Frequently Asked Questions. Retrieved From: https://eczemahelp.ca/resources/





Leave a Comment